The risk of death depends on type of stroke. Transient
Ischaemic Attack (TIA) has the best outcome followed by stroke caused by
carotid stenosis. The blockage of any artery with rupture of cerebral blood
vessel is the most dangerous of all. Hypertension in this hospital based study
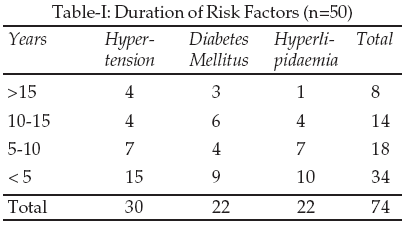
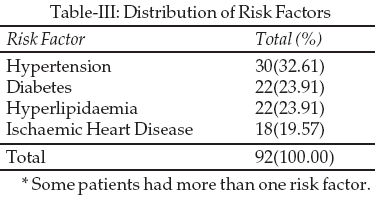
was the most common risk factor for stroke which was present in 32.61% of the
whole sampling.21-23
The findings are similar to that reported by Lickner H (40.06%).24
Diabetes was the second most important risk factor present in 23.91% of
patients.25,26
These findings correlate with findings of Basharat RA27
(21%) and Liaquat A (27%).28
Hyperlipidaemia was found in twenty-two (23.91%) of patients and was the 3rd
most common risk factor for stroke in this study which is similar to those
reported by Tanveer A (16%).29
Ischaemic heart disease was fourth most common risk factor of stroke in 19.57%
of patients.30-32
1. World Health Organisation. Cerebrovascular Disorders
(Offset Publications). Geneva: World Health Organization. ISBN 9241700432
1978.
2. Hebert PR, Gaziano JM, Chan KS. Cholesterol lowering
with statins drugs. Risk of stroke, and total mortality. An overview of
randomized trials. JAMA 1997;278(4):313-21.
3. Goldstein LB, Adams R, Becker K. Primary prevention of
Ischaemic Stroke. AHA Scientific Statement. Circulation 2001;103:163-82.
4. Clark CM, Perry RC. Type II diabetes and macrovascular
disease. Epidemiology and etiology. Am Heart J 1999;138:930-3.
5. Elkind MS, Sacco RL. Stroke risk factors and stroke
prevention. Semi Neurol 1998;18:429-39.
6. Hu FB, Manson JE, Stampfer MJ. Diet, lifestyle, and the
risk of type 2 diabetes mellitus in women. N Engl J Med 2001;345:790-797.
7. Hasan SR, Ghouri ASK. Frequency of known risk factors of
stroke and its outcome in patients admitted in Sindh Government Qatar Hospital
Karachi. Pak J Med Sci 2007;23(4):634-6.
8. Rafique BA, Yousuf M, Iqbal J, Khan MM. Frequency of
known risk factors for stroke in poor patients admitted to Lahore General
Hospital in 2000. Pak J Med Sci 2002;18:280-3.
9. Khan J. Frequency of hypertension in stroke patients
presenting at Ayub Teaching Hospital. J Ayub Med Coll Abbottabad
2006;18(1):36-9.
10. Iqbal F, Hussain S, Hassan M. Hypertension, diabetes
mellitus and hypercholesterolaemia as risk factors for stroke. Pak J Med Res
2003;42(1):17-22.
11. Westin S. Thresholds for normal blood pressure and
serum cholesterol. BMJ 2005;330:1461-62.
12. He J, Whelton PK. Epidemiology and prevention of
hypertension. Med Clin North Am 1997;81:1077.
13. The sixth report of the joint National Committee on
Prevention, Detection, Evaluation and treatment of high blood pressure. Arch
Intern Med 1997;157:2413-45.
14. Expert panel on Detection, Evaluation and Treatment of
high Blood Cholesterol in Adults. Executive summary of the third report of the
National Cholesterol Education program (NCEP) Expert panel on
Detection, Evaluation and Treatment of high Blood Cholesterol in Adults
(Adults treatment panel III) JAMA 2001;285:2486-96.
15. Meyer JS, Rogers RL, Mortel KF, Judd BW. Hyperlipidemia
is a risk factor for decreased cerebral perfusion and stroke. Arch Neurol
1987;44(4):418-22.
16. Iso HJ Jr, Wentworth D. Serum cholesterol levels and
six year mortality from stroke in 360,977 men screened for the multiple risk
factors intervention trial. N Engl J Med 1989;320:904-10.
17. Schwartz SM, Reidy MA. Factors important in arterial
narrowing. J Hyperten Suppl 1996;14(5):S71-81.
18. Stampfer MJ, Hu FB, Manson JE, Rimm EB, Willett WC.
Primary prevention of coronary heart disease in women through diet and
lifestyle. N Engl J Med 2000;343:16-22.
19. Safeer M, Tariq M, Rehman U. Frequency of risk factors
of cerebral infarction in stroke patients. A study of 100 cases in Naseer
Teaching Hospital, Peshawar. Pak J Med Sci 2008;24(1):109-13.
20. Aho K, Harmsen P, Hateno S, Maarqyardsen T, Smirnov VE,
Strasser T. On behalf of the participants in the W.H.O collaborative study on
control of stroke in the community. Cerebrovascular diseases in the community.
Results of the W.H.O collaborative study. Bulletin of W.H.O 1998;58:113-30.
21. Basharat RA, Yousuf M, Iqbal J, Khan MM. Frequency of
known risk factors for Stroke in poor patients admitted to Lahore General
Hospital in 2000. Pak J Med Sci 2002;18(4):280-3.
22. Khan H, Afridi AK, Ashraf S. A hospital based study on
stratification of risk factors of stroke in Peshawar. Pak J Med Sci
2006;22(3):304-7.
23. Khan SN, Vohra EA. Risk factors for stroke: A hospital
based study. Pak J Med Sci 2007;23(1):17-22.
24. Lickener H, Eiswarth CC, Hachinski VC. Risk factors for
stroke in Australian population. Wien Klin Wochensher 1993;105(14):393-403.
25. Kuller LH, Dorman JS, Wolf PA. Cerebrovascular disease
and diabetes. Chapter XVIII in Diabetes in America, Harris MI, Hamman RF, eds.
NIH publ 1985;85-1468.
26. Abbott RD, Donahue RP, MacMahon SW, Reed DM, Yano K.
Diabetes and the risk of stroke. The Honolulu Heart Program. JAMA
1987;257:949-52.
27. Basharat RA, Elahi A, Tariq M, Saeed A. One month audit
of stroke at PIMS. Pak J Neurol 1999;56(1):12-5.
28. Liaqat A, Jamil H, Alam MS. Risk factors in stroke. J
Coll Physician Surg Pak 1996;7:7-10.
29. Tanveer A. Localization and management in
Cerebrovascular accident: A comparison of clinical assessment versus C.T Scan
(Dissertation). J Coll Physician Surg Pak 1996;5-6.
30. Ali L, Jameel H, Shah MA. Risk factors in stroke. J
Coll Physicians Surg Pak 1997;7:7-10.
31. Javed MA, Ahmed M, Sial MSH, Naheed T. Risk factors in
stroke. Pak J Neurol 1998;4:55-8.
32. Alam I, Haider I, Wahab F, Khan W, Taqweem MA,
Nowsherwan. Risk factors stratification in 100 patients of acute stroke. J
Postgrad Med Ins 2004;18(4):583-91.
33. Skafor ET, Lethell HO, Salinin KT, Aberg H. Doantihypertensive drugs
precipitate diabetes inpredisposed men? BMJ 1989;298:1147-52.