|
|
||||
|
Published by : PROFESSIONAL MEDICAL PUBLICATIONS |
||||
|
ISSN 1681-715X |
||||
|
||||
|
- |
||||
|
CASE REPORT |
||||
|
- |
||||
|
Volume 24 |
July - September 2008 |
Number 4 |
||
|
|
||||
|
|
||||
|
|
||||
|
Published by : PROFESSIONAL MEDICAL PUBLICATIONS |
||||
|
ISSN 1681-715X |
||||
|
||||
|
- |
||||
|
CASE REPORT |
||||
|
- |
||||
|
Volume 24 |
July - September 2008 |
Number 4 |
||
|
|
||||
|
|
||||
Spontaneous resolution of
Non-immune Hydrops fetalis
Habiba Sharaf Ali1
Abstract
A case report of hydrops fetalis characterized by ascites and scalp edema of unknown etiology is described. The hydrops developed at 24 weeks and resolved completely without treatment resulting in a live born infant at term.
KEY WORDS: Hydrops Fetalis.
Pak J Med Sci July - September 2008 Vol. 24 No. 4 621-623
How to cite this article:
Ali HS. Spontaneous resolution of Non- immune Hydrops fetalis. Pak J Med Sci 2008;24(4):621-3.
1. Dr. Habiba Sharaf Ali,
Associate Professor,
Obstetrics and Gynecology,
Ziauddin University,
Karachi – Pakistan.
Correspondence
Dr. Habiba Sharaf Ali
A- 705, Chapel Ocean Centre,
Block-4, Clifton, Karachi.
E-mail: rabel5@yahoo.com
* Received for Publication: February 19, 2008
* Accepted: June 27, 2008
INTRODUCTION
Hydrops fetalis is a serious fetal condition defined as the presence of excess fluid in more than one body compartment. The fluid should present in any of the following two cavities to be diagnose hydrops fetalis e.g. subcutaneous tissues, lung, abdominal cavity and pericardial cavity.
1 The incidence of hydrops is difficult to ascertain as most of the fetuses die early in pregnancy. However in USA its incidence is approximately one in 600 to one in 4000.1 In Southeast Asia it is more common and its incidence varies from one in 500 to one in 1500.2 It may be of two types immune due to maternal hemolytic disease or non immune due to any other cause. With the use of Anti D prophylaxis immunological causes account for less than 20% cases.1 More common are non immune causes of hydrops fetalis.There are more than 80% conditions associated with it such as chromosomal abnormality, structural cardiovascular disease, cardiac rhythm disorders, chest anomaly, hematological disease and infection.
3 As hydrops fetalis has poor prognosis most of the obstetrician consider termination of pregnancy. The prognosis is even poorer if hydrops fetalis is diagnosed in first half of pregnancy.3 This report describes a case of severe hydrops fetalis unknown etiology diagnosed at 24 week of gestation with complete resolution in third trimester without intrauterine treatment and with uncompleted neonatal outcome.CASE REPORT
A 22 year old woman Para 1+0 last delivery by Caesarean section due to non progress of labour came for booking at 12 weeks gestation. Routine ultrasound scan at that time was normal. A repeat scan at 24 weeks gestation showed gross ascites and scalp edema, bilateral pleural effusion and ventricular dilatation. There was no pericardial effusion. Fetal biometry was consistent with the menstrual dates and fetal heart rate and rhythm was normal. A detailed fetal examination was performed. Growth parameter showed an abnormally enlarged abdomen. No other fetal abnormality was seen. The placenta was anterior and normal in size. The maternal blood group was "B" positive.

A viral screening had revealed no evidence of recent maternal infection with toxoplasmosis, rubella, cytomegalovirus or herpes simplex. IgG & an IgM level for human parvovirus was also normal. All other investigations were normal. At 34 weeks a further ultrasound measurement was undertaken. The fetal ascites and scalp edema and pleural effusion resolved completely. A further scan at 36 weeks revealed a completely normal looking fetus. Due to her previous Caesarean section we waited for spontaneous labour which started at 39 weeks and patient delivered an alive normal male child weighing 3.2kg spontaneously with good Apgar score.
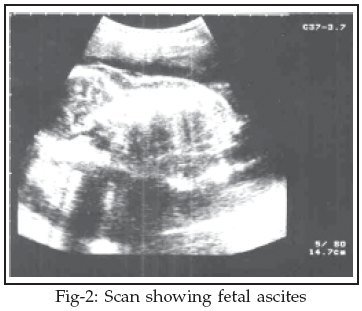
Discussion
In general Non Immune Hydrops Fetalis is regarded to have poor prognosis and usually termination of pregnancy is advised.
4 Non immune hydrops can occur at any time during pregnancy. There is no standard treatment. People are treating non immune Hydrops Fetalis with intrauterine transfusion in case of human parvovirus infection, shunting or open surgery in case of extra lobular lung sequestration associated with fetal hydrops and maternal digitalization.1 In our case as the etiology was unknown, no intervention was carried out. Very few cases of complete resolution of hydrops fetalis of unknown etiology are described in literature. Henrich1 described complete resolution of severe non-immune Hydrops fetalis in second trimester. Swin et al,5 described survival of two cases of hydrops of idiopathic etiology. Spontaneous resolution of non-immune hydrops resulting from parvovirus infection has been reported by numerous investigators and John Rodie6 describes spontaneous resolution of 34% of non-immune hydrops resulting from parvovirus B19. Boris M7 also described the cases of spontaneous resolution of Hydrops fetalis from parvovirus. Similarly Teresa et al8 has described spontaneous resolution of hydrops fetalis, secondary to parvovirus infection presented early in pregnancy. P.S Bhal9 presented a case of spontaneous resolution of non immune hydrops fetalis secondary to .transplacental pavovirus B19 infection. This case together with other reports would suggest that hydrops is not a preterminal event and may resolve spontaneously particularly if there are no signs of associated congenital malformations, chromosomal aberrations, intrauterine infections or trauma are observed.1 As such one could say that a hydrops showing signs of resolution can be managed conservatively.REFERENCES
1. Henrich W, Heeger J, Schmider A, Dudenhausen JW. Complete spontaneous resolution of severe no immunological hydrops fetalis with unknown etiology in the second trimester – A case report. J Perinat Med 2002;30:522–7.
2. Hamdan AH. Hydrops Fetalis, eMedicine 22, 2006.
3. Ericgauniaux IJ. Outcome of NIHF diagnosed during the first half of pregnancy. Obstet Gynae 1997;90:321-5.
4. Rodis JF, Quinn DL, Gary GW Jr. Anderson LJ, Rosengren S, Cartter ML, et al. Management and outcomes of pregnancies complicated by human B19 parvovirus infection: A prospective study. Am J Obstet Gynecol 1990;163:1168-71.
5. Swain S, Cameron AD, McNay MB, Howatson AG. Prenatal diagnosis and management of non immunological hydrops fetalis. Aust NZJ Obstet Gynaecol 1999;39:285.
6. Rodis JF, Borgida AF, Wilson M, James B, Egan FX, Leo MV, et al. Campbell. Management of parvovirus infection in pregnancy and outcomes of hydrops. A survey of members of the Society of Perinatal Obstetricians. Am J Obstet Gynecol 1998;179:984-8.
7. Petrikovskdya BM Baker, Schneid. Fetal Hydrops Secondary to human parvovirus infection in early pregnancy. Prenatal Diagnosis 1996;16:342-4.
8. Kelly T, Mathers A. Early presentation and spontaneous resolution of hydrops Fetalis, secondary to parvovirus B19 infection. J Obstet Gynaecol 1998;18:190-1.
9. Bhal PS, Davies NJ, Westmoreland D, Jones A. Spontaneous resolution of No immune hydrops fetalis secondary to transplacental parvovirus B19 Infection. Ultrasound Obstet Gynaecol 1997;55-7.
HOME | SEARCH | CURRENT ISSUE | PAST ISSUES
Professional
Medical Publications
Room No. 522, 5th Floor, Panorama Centre
Building No. 2, P.O. Box 8766, Saddar, Karachi - Pakistan.
Phones : 5688791, 5689285 Fax : 5689860
pjms@pjms.com.pk