|
|
||||
|
Published by : PROFESSIONAL MEDICAL PUBLICATIONS |
||||
|
ISSN 1681-715X |
||||
|
||||
|
- |
||||
|
ORIGINAL ARTICLE |
||||
|
- |
||||
|
Volume 24 |
October - December 2008 (Part-II) |
Number 6 |
||
|
|
||||
|
|
||||
|
|
||||
|
Published by : PROFESSIONAL MEDICAL PUBLICATIONS |
||||
|
ISSN 1681-715X |
||||
|
||||
|
- |
||||
|
ORIGINAL ARTICLE |
||||
|
- |
||||
|
Volume 24 |
October - December 2008 (Part-II) |
Number 6 |
||
|
|
||||
|
|
||||
Study of anxiety and depression
during pregnancy
Fareeha Hamid1, Aftab Asif 2, Imran Ijaz Haider3
ABSTRACT
Objectives: To find out the prevalence of anxiety and depression symptoms during pregnancy.
Methodology: The sample of one hundred pregnant women was screened while waiting for their prenatal visit in obstetric clinic of FMH (Fatima Memorial Hospital). They were eligible for the study if they were pregnant and giving consent. Control group (n=100) was taken from non pregnant women matched on age, education, marital status and monthly income. This was cross-sectional study and the convenience sampling (non-probability sampling) technique was used. The study was spread over the period of six months. A brief questionnaire for collecting demographic information was used. DSM-IV criteria for assessing past psychiatric illness were also used by the researcher. HADS (Hospital Anxiety & Depression scale) was used to assess anxiety & depressive symptoms.
Results: Of one hundred pregnant women 39% & 18% scored above cut-off on anxiety and depression scale respectively. Among control group the percentage for anxiety & depression was 28% & 12% respectively. Seventeen percent of pregnant women reported receiving psychiatric (pharmacological or psychotherapy) treatment for psychological issues. The T-test results showed significant difference between two groups regarding anxiety and depression.
Conclusions: Pregnant women experience more anxiety & depression as compared to their closely matched counterparts and most of them are not being monitored during this time. More work is needed for detection, referral and treatment of anxiety/ depression during pregnancy. Clinical studies for maternal mental health & fetal consequences are also needed.
KEY WORDS: Pregnancy, Depression, Anxiety.
Pak J Med Sci October - December 2008 (Part-II) Vol. 24 No. 6 861-864
How to cite this article:
Hamid F, Asif A, Haider II. Study of anxiety and depression during pregnancy. Pak J Med Sci 2008;24(6):861-64.
1. Ms. Fareeha Hamid, ADCP, MSc.
Clinical Psychologist,
Department of Psychiatry & Behavioral Sciences,
2. Dr. Aftab Asif, MRC Psych., MBBS
Associate Professor, Dept. of Psychiatry,
Ganga Ram Hospital, Lahore.
3. Dr. Imran Ijaz Haider, MRC Psych., D.P.M., MBBS,
Assistant Professor & Head,
1-3: Department of Psychiatry & Behavioral Sciences,
Fatima Memorial Hospital College of Medicine & Dentistry,
Lahore - Pakistan.
Correspondence
Ms. Fareeha Hamid,
Email: rayofhope786@hotmail.com
* Received for Publication: March 8, 2008
* Revision Received: September 17, 2008
* Final Revision Accepted: September 20th 2008
INTRODUCTION
Pregnancy is a time of growth and hope, but it is also a time when woman is very vulnerable. Psychologically healthy woman often find a pregnancy a means of self-realization. Other women use pregnancy to diminish self-doubts about feminity or to reassure that they can function as women in the most basic sense. Still others view pregnancy negatively; they may fear childbirth or feel inadequate about mothering. At least one in ten mothers in all levels of society, and regardless of socioeconomic conditions experience clinical depression and/or anxiety before and up to a year after childbirth. The trimesters can bring their characteristic challenges and rewards, the nausea, fatigue & emotionality. For many women, the first and third trimesters are difficult.
1Approximately 21% of women experience a mood disorder and 30% anxiety disorder at some points in their lives.
2 Although historically it was believed that pregnant women are at lower risk of anxiety and mood disorders, 3 but recent studies don’t support this belief. Rather between 10 and 27% of women experience depressive symptoms during pregnancy, including 2-11% who experience major depressive disorder.According to a study, 23% of pregnant women receiving prenatal care in California demonstrated depressive & anxiety disorders. In the studies including poor pregnant women the rate of maternal depression ranges from 30-70%. This empirical data substantiate that mood state, neuro-endocrine & immune systems may play a critical role in reproductive outcome and fetal development.
4Studies have also identified that anxiety and stress have a role in altering the duration of pregnancy & the well being of the fetal brain. One group of researchers, report a study at 32 weeks gestation to see if there was any correlation between anxiety and uterine blood flow. The results showed that, in the high anxiety mothers, there was impaired blood flow through uterine arteries. The reduced uterine blood flow could be a mechanism for lower birth weight, preterm birth and infants with elevated cortisol seen in highly anxious women.
5 Another group from Sweden reported less cerebral blood flow in instances of increased maternal anxiety.6 These findings reveal that antenatal anxiety occur frequently, overlaps with depression and increase the likelihood of postnatal depression.The aim of present research was to detect the prevalence of anxiety and depression in pregnant women in order to grasp the attention of health care system by monitoring such psychological issues and to help them to deal with the burden of anxiety and depression. Based on previous findings it could be hypothesized that anxiety and depression phenomenon would be prevalent during pregnancy.
METHODOLOGY
The present research recruited a sample of on hundred participants. They included pregnant women coming to obstetric clinics for their prenatal checkup. Sample for control group was taken from non pregnant women by matching on age, education, and marital-status and monthly income. This was a cross-sectional study and the sampling technique was of convenience sampling. The study was spread over the period of six months. Pilot study was conducted on five participants and informed consent was taken by each participant.
A standardized tool, HADS
7 (Hospital Anxiety and Depression scale), was used. This is basically 14-item self-report valid scale, designed to briefly measure current anxiety & depression symptomatology. Before administering HADS, the participants were asked to fill in a brief demographic form. DSM-IV8 criteria for assessing the past psychiatric illness were also used by the researcher. Owing to a low level of literacy among some participant, the researcher read out the questionnaire and noted their responses.
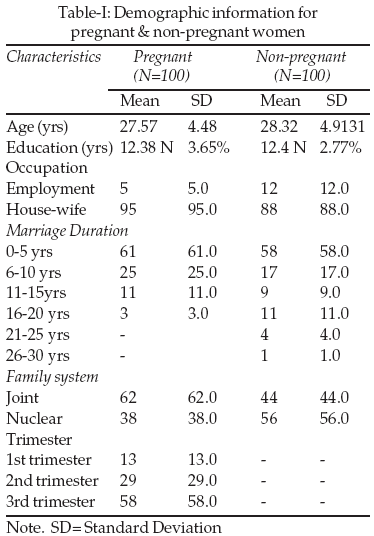
Thirteen women (13%) were seen during first trimester, twenty nine (29%) during the second trimester and fifty eight (58%) during third trimester.
Results
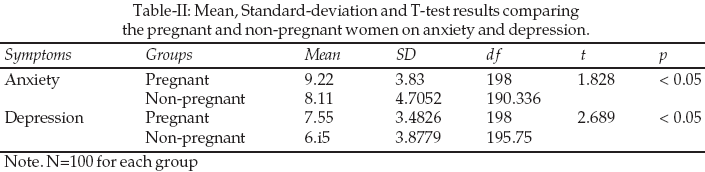
The results given in Table-II indicate significant difference between the scores of pregnant women on the scale of anxiety (9.22) and on the scale of depression (7.55) as compared to non-pregnant women.
DISCUSSION
Our findings showed that anxiety and depression symptoms are common in pregnant women than among closely matched controls. The results obtained appear to strongly reaffirm earlier findings of various researchers and clinicians working in this area.
1,2,6Kelly
4 reported that 23% of pregnant women receiving prenatal care in California demonstrated anxiety and depressive disorder. Megan et al9 performed a study to assess rates of detection and treatment of minor and major depressive disorder, panic disorder and post traumatic stress disorder among pregnant women receiving prenatal care at public sector obstetric clinics. After the visit, patients were asked whether their clinician recognized a mood or anxiety disorder. Medical records were reviewed for documentation of psychiatric illness and treatment. Results revealed that 26% of patients who screened positive for a psychiatric illness were recognized as having mood or anxiety disorder by their health care providers. Moreover, clinicians detected disorders among 12% of patients who showed evidence of suicidal ideation. In our study, 39% women scored positive for anxiety and 18% scored positive for depression.The patients questionnaires showed that among women with anxiety and depression ten (17%) were identified or referred for psychiatric treatment during their pre-natal visit.
The low detection and referral rates for depression among pregnant females may be a result of number of factors. Clinicians may be reluctant to ask questions and patients may avoid reporting problems that arise from depression or anxiety. Symptoms of depression during pregnancy may not raise clinicians or patients concern because several of these experiences e.g., disturbance in appetite, sleep and energy levels are normative for many pregnant women.
10Other possible contributions include time-constraints, referral limitations and provider education and training. Large survey studies have shown that majority of obstetric-gynecologic residents neither received training about clinical depression during their residency (80%), nor completed a continuing medical education course on the treatment of clinical depression among women (60%).
11 Approximately 50% of obstetrician-gynecologists cite incomplete knowledge of diagnostic criteria as a barrier of identification of depression.12The expectation that obstetrician and gynecologist will diagnose and treat common mental health disorders is of recent origin, and many providers may not think that it should be part of their clinical responsibilities.
The information revealed from present research may be used to justify systematic screening for anxiety and depression in clinical encounter with pregnant women as a first step in determining which women may require further treatment for their mood symptoms. An elevation in anxiety/depression symptoms has been associated with adverse maternal and infant outcomes. This has been revealed by earlier findings.
5,6Importantly the effect of anxiety affected the fetus more than any other factor, including smoking during pregnancy, low birth weight or anxiety of mother. In the present research, the detection of antenatal anxiety and depression and not its effect on newborn was the f ocus of study.
Clinical implications & Limitations:
*
Anxiety/ depression in pregnancy could have long-term effects on children’s behavioral / emotional problems.*
Long-term alterations in the stress response could be influenced by early, even antenatal experience.*
Reducing maternal anxiety in pregnancy could have protective effect in new born.Limitations of the study: Data on maternal anxiety & depression was based on self-report questionnaires. Questionnaire was orally administered with few women considering their low literacy rate.
CONCLUSIONS
High prevalence of anxiety and depression symptoms during pregnancy indicate that women in childbearing years could be vulnerable to anxiety and depressive disorder. It is suggested that physicians in all patient care specialties need to be familiar with the prevalence and course of these disorders, particularly during pregnancy & post-partum period. The obstetrician should regularly test for anxiety and depression with simple means from the very first moment of planning for a child and should use the test results for pregnancy mood profile. The profile could assist in determining the risk of postpartum depression & serve as an early alert for postpartum suicide.
The evidence from this & other studies, however, provide an impetus for developing prevention, intervention & support programs for highly anxious & depressed pregnant women. These programs could include stress reduction, instruction as well as treatment to reduce anxiety & neuro-endocrine reactions to the stress throughout pregnancy, or even after conception. The benefits of implementing good mental health in antenatal care may have long lasting benefits for the mother, infant and family.
REFERENCES
1. Saddock K. Synopsis of Psychiatry. Behavioral Sciences and Clinical Psychiatry.9th edition. Lippincott Williams & Wilkins USA 2003.
2. Kessler R, Mc Gonagle K, Zhao S. Lifetime and 12 months’ prevalence of DSM-III-R Psychiatric Disorders in the United States: Results from the National Co morbidity survey. ArchiGen Psychiatry 1994;51:8-19 (Abstract)
3. O’Hara MW, Zekoski EM, Philipps LH. Controlled prospective study of postpartum mood disorders: comparison of childbearing women. J Abnormal Psych 1990;99:3-15.
4. Kelly RH, Russo J, Katon W. Somatic complaints among pregnant women cared for in obstetrics: normal pregnancy or depressive and anxiety symptom amplification revisited. Gen Hosp Psychiatry 2001;23(3):107-13.
5. Teixeria JM, Fisk NM, Glover V. Association between maternal anxiety in pregnancy and increased uterine artery resistance index: cohort based study. BMJ 1999;318(7193):1288-9.
6. Sjostrom K, Valentin L, Thelin T, Marsal K. Maternal anxiety in late pregnancy and fetal heodynamics. Eur J Obstet Gynecol Reprod Biol 1997;74(2):149-55.
7. Zigmond AS, Snaith RP. The Hospital Anxiety & Depression Scale. Acta Psychiatr Scand 1983;67:361-70.
8. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition. Washington, DC: American Psychiatric Association 1994.
9. Megan V, Robert A, Mary A. Screening for and detection of Depression, Panic Disorder & PTSD in public sector Obstetric clinics. Psychiatric Service 2004;55:407-14.
10. Klein MH, Essex MJ. Pregnant or Depressed? The effect of overlap between symptoms of depression & somatic complaints of pregnancy on rates of major depression in the second trimester. Depression 1995;2:308-14.
11. Marcus S, Flynn H, Blow F. Depressive symptoms among pregnant women screened in obstetric settings. J Women Health 2003;12:373-80.
12. Heron J, Thomas G, O’ Conner. The course of anxiety and depression through pregnancy and postpartum in a community sample. J Affective Disorders 2004;80:65-73.
HOME | SEARCH | CURRENT ISSUE | PAST ISSUES
Professional
Medical Publications
Room No. 522, 5th Floor, Panorama Centre
Building No. 2, P.O. Box 8766, Saddar, Karachi - Pakistan.
Phones : 5688791, 5689285 Fax : 5689860
pjms@pjms.com.pk