|
|
||||
|
Published by : PROFESSIONAL MEDICAL PUBLICATIONS |
||||
|
ISSN 1681-715X |
||||
|
||||
|
- |
||||
|
ORIGINAL ARTICLE |
||||
|
- |
||||
|
Volume 25 |
July - September 2009 |
Number 4 |
||
|
|
||||
|
|
||||
|
|
||||
|
Published by : PROFESSIONAL MEDICAL PUBLICATIONS |
||||
|
ISSN 1681-715X |
||||
|
||||
|
- |
||||
|
ORIGINAL ARTICLE |
||||
|
- |
||||
|
Volume 25 |
July - September 2009 |
Number 4 |
||
|
|
||||
|
|
||||
Allopurinol as an adjuvant therapy
for refractory schizophrenia
Arasteh Modabber1, Sanobar Tahaie Najmedin Pharm D2
ABSTRACT
Objective: This study was conducted to investigate the effect of allopurinol in the treatment of chronic refractory schizophrenia.
Methodology: This is a double blind cross-over Randomized Clinical Trial. Nineteen schizophrenic cases in two groups is quite a low number to arrive at meaningful conclusion. Patients were grouped in allopurinol and placebo group by randomized blocking method. The evaluation of symptoms was done by Positive and Negative Syndrome Scale (PANSS) questionnaire at 0, 3, 6, 9 and 12 months and one year after the cessation of drug consumption. The data was analyzed by paired T test and Mann-Whitney U test.
Results: There was a significant decrease in positive, general and total symptoms’ scores in patients who took allopurinol for first six month in comparison to their baseline score at beginning of the study (P<0.05). Finally, positive, negative, general and total score had no significant difference between allopurinol and placebo treatment (P>0.05).
Conclusion: Our study shows some degree of decrease (but not significant) in symptoms scores. It seems that more studies with a larger sample size, different doses of allopurinol and different group of patients are necessary in high refractory schizophrenic patients to come at some meaningful conclusions.
KEY WORDS: Chronic schizophrenia, Allopurinol, Adenosine.
Pak J Med Sci July - September 2009 Vol. 25 No. 4 591-596
How to cite this article:
Modabber A, Pharm STND. Allopurinol as an adjuvant therapy for refractory schizophrenia. Pak J Med Sci 2009;25(4):591-596.
1. Arasteh Modabber MD,
Assistant Professor of Psychiatry Department,
Kurdistan University of Medical Sciences,
Pasdaran Str,
Psychiatry Hospital,
Sanandaj, Iran.
2. Sanobar Tahaie Najmedin,
Pharmacist,
Faculty of Medicine,
Kurdistan University of Medical Sciences,
Sanandaj, Iran.
Correspondence
Arasteh Modabber,
Email: m_araste2007@yahoo.com
* Received for Publication: October 14, 2008
* Revision Received: October 21, 2008
* 2nd Revision Received: June 11, 2009
* Final Revision Accepted: June 21, 2009
INTRODUCTION
In spite of availability of GABA
*ergic drugs during the last decades, resistance to them1 and dopamine receptor blockers in 30% of patients2, suggest a defect in other inhibitory mechanisms in schizophrenia, especially the effect of adenosine as an effective factor is considerable.Adenosine has an immunomodulatory role on dopamine and glutamate systems via effects on A2 and A2A receptors, suggests the hypothesis about adenosine role in inhibitory defects of schizophrenia. Adenosine agonists block the glutamate release and cause hyperpolarization of brains’ post ganglia neurons via A2 receptors, inhibition of brain stimulations and blocking the NMDA receptors’ function. Finally, they could decrease the schizophrenia symptoms.
3Allopurinol is a xanthine oxidase inhibitor, routinely used in gout treatment, and also earlier studies have suggested its potential effect in mania
4, and dementia5. Allopurinol, as an augmentation treatment in schizophrenia, based on its effect on adenosine, has significant results in a few studies in recent years.6-8In two earlier studies, the duration of study was eight week.
7,8 One of the limitations in Brunstein et al7 study was the short course of study and they suggested the possibility of the continuation of allopurinol effect in placebo phase in some patients.In reported studies, prolonged treatment with allopurinol and prolonged follow up of patients after allopurinol treatment have not been studied, therefore this study was designed to investigate allopurinol augmentation therapy in chronic refractory schizophrenia.
METHODOLOGY
This investigation was a double blind cross-over RCT. We studied all schizophrenic patients in the chronic psychiatry caring center in Sanandaj city of Iran during 2003-2006. All patients in this center with definite schizophrenia based on DSM-IV TR criteria were 38, but only 19 patients who had eligible criteria were included in the study. Inclusions criteria were: 1) Refraction to antipsychotic doses equivalent 1000 mg chlorpromazine during six month in two courses, with two different classes of drugs,
9 2) No appropriate function in five past years or from onset of disease. 3) PANSS score at least 50 before starting the study. 4) No significant difference between PANSS scores one year before the study and in the beginning of the trial.During the study, treatment with other drugs, like antidepressants, benzodiazepines, and mood stabilizers was continued. Hematologic tests, liver and renal function tests, and Uric acid levels were done before the study and every six months during the study. The patients who had other psychotic, neurological and medical diseases and were experiencing drugs side effects were excluded from the study.
Informed consent was obtained from local warden court (because the most of our samples are incapable and did not have any family supervisor) and the study was approved by ethical committee of Kurdistan University of Medical Sciences. The trail was performed in accordance with the Declaration of Helsinki and subsequent revisions (World Medical Association Declaration of Helsinki, 2000).
Patients based on randomized blocking allocation were divided into two groups: intervention (ten patients) and placebo (nine patients). Allopurinol 300 mg bid, in intervention group and placebo (300 mg bid) was added to the standard treatment in two groups. Treatment was continued for six months and after two weeks washout period, the cross-over treatment was done and treatment was continued for another six months period. After twelve months, the allopurinol and placebo capsules in two groups were discontinued. The evaluation of symptoms was done by PANSS questionnaire in 0, 3, 6, 9, 12 months and one year after the cessation of drug consumption. During the study all patients were treated with their standard drugs, and symptoms and side effects of drugs were evaluated.
We considered the changes in the mean PANSS score compared to month zero for first phase and month six for second phase of the study as response to schizophrenia treatment. Throughout the study, the rater and the patients were blind to assignments. Mann-Whitney U test and paired t test was used for data analysis.
RESULTS
Nineteen patients were studied. Two of patients starting on placebo were excluded from the study, one of them in intervention phase because of loss of consciousness though its relation to allopurinol was not proved. The other was excluded due to the request of the patient’s family. We followed up 17 patients until the end of the study.
There was no significant difference between two groups in the beginning of the study (Table-I).
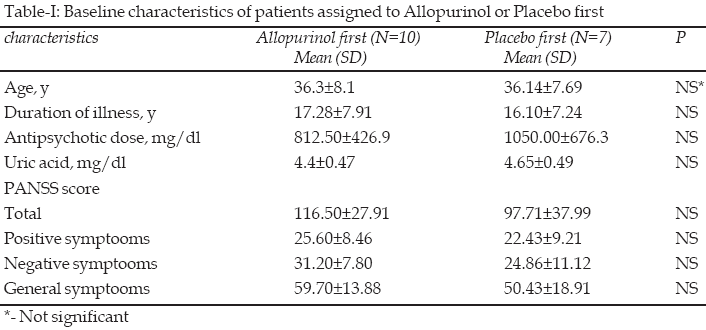
From 17 patients, six patients were also being treated with benzodiazepines, four with antidepressants and five were being treated with mood stabilizers. There was no significant difference in positive, negative, general and total PANSS test scores between allopurinol and placebo treatment in different times (p>0.05).
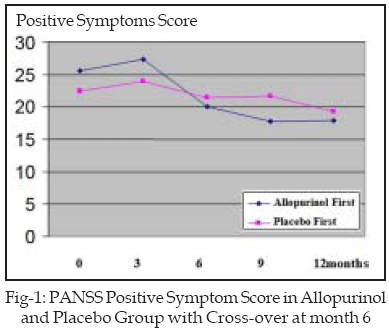
There was no significant difference in the positive symptoms mean score in the group starting on placebo at the first phase and after cross-over to allopurinol (p>0.05). one year after the end of the study, positive symptoms mean score in this group had no significant difference with beginning of the study, sixth month, and twelfth month (p>0.05).
The positive symptoms mean score in the group starting on allopurinol had a significant difference in sixth month of the study (20.10±4.74) compared with onset of the study (25.6±8.46) (p=0.02, t=2.59). But after cross-over in this patients positive symptoms mean score at twelfth month of the study (17.90±3.07) had no significant difference with sixth month of the study (p=0.22, t=1.31) Figure-1. One year after the end of the study, positive symptoms mean score in this group had no significant difference in the beginning of the study, sixth month, and twelfth month (p>0.05).
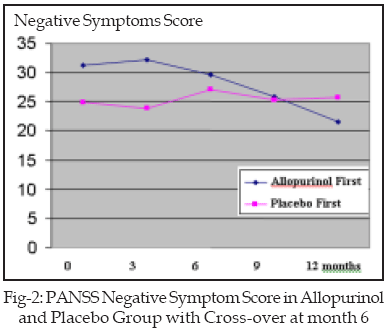
There was no significant difference in the negative symptoms mean score in the group starting on placebo, at the first phase and after cross-over to allopurinol (p>0.05). But the difference between one year after the end of intervention (20.10±8.22) and sixth month (27.00±13.14) (p=0.01, t=3.49) and twelfth month (25.71±12.02) was significant (p=0.01, t=3.48).
There was no significant difference in the negative symptoms mean score in the group starting on allopurinol at the first phase of the study. After cross-over, there was a significant difference in negative symptoms mean score in the twelfth month (21.6±5.52) in comparison with the sixth month (29.6±7.98) (p=0.004, t=3.9) Figure-2. One year after the termination of the intervention, negative symptoms mean score (17.5±7.73) had a significant difference compared with the beginning of the study (37.2±7.8) (p=0.000, t=9.42) and the sixth month (29.6±7.98) (p=0.00, t=7.33), but there was no difference in comparison with twelfth month (21.6±5.52) (p=0.13, t=1.62).
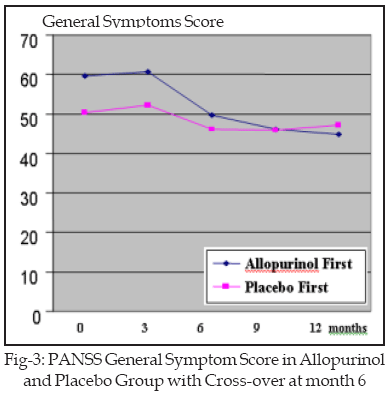
There was no significant difference in the general symptoms mean score in the group starting placebo at the first phase and after cross-over to allopurinol (p>0.05). One year after the end of the study, general symptoms mean score in this group (35.86±12.36) had a significant difference in comparison with onset of the study (50.43±18.91) (p=0.004, t=4.49), the sixth month (46.00±16.97) (p=0.03, t=2.81) and the twelfth month of the study (47.14±16.51) (p=0.02, t=3.1).
General symptoms mean score, in the group which first received allopurinol, had a significant difference in the sixth month (49.6±9.8) compared with beginning of the study (59.7±13.88) (p=0.01, t=3.17). After cross-over, there was a significant difference in general symptoms mean score in the twelfth month (44.9±7.18) compared with the sixth month (49.6±9.8) (p=0.02, t=2.81) Figure-3. One year after the end of intervention, the general symptoms mean score, in this group (33.6±9.04) had a significant difference compared with beginning of the study (59.7±13.88) (p=0.000, t=7.98), the sixth month (49.6±9.8) (p=0.001, t=4.58) and the twelfth month (44.9±7.18) (p=0.004, t=3.79).
The total mean score by PANSS questionnaire in the group starting on placebo, had no significant difference at the first phase and after cross-over to allopurinol (p>0.05). One year after the end of intervention there was a significant difference in the total mean score between this group (74.85±25.91) and the onset of the study (97.91±37.99) (p=0.02, t=3.02), the sixth month (94.42±32.25) (p=0.005, t=4.34) and the twelfth month of the study (92.14±34.63) (p=0.02, t=3.15).
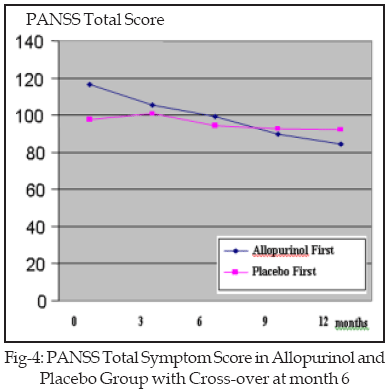
The total mean score by PANSS questionnaire, in the group starting on allopurinol, had a significant difference in the sixth month of the study (99.3±19.98) compared with the beginning of the study (116.5±27.91) (p=0.01, t=2.84). After cross-over, the total means score in this group, had a significant difference in the twelfth month of the study (84.4±12.25) compared with sixth month (99.3±19.98) (p=0.007, t=3.44) Figure-4. One year after the end of intervention, the total mean score in this group (71.2±14.42) had a significant difference compared with beginning of the study (116.5±27.91) (p=0.000, t=7.09), the sixth month (99.3±19.98) (p=0.000, t=5.53), and the twelfth month of the study (84.4±12.25) (p=0.000, t=5.68). The changes in the mean scores, by PANSS questionnaire have been illustrated in Figures 1-4.
DISCUSSION
The results of this study, showed no significant difference in PANSS mean scores between allopurinol and placebo treatment in all the phases of the study. Although, the patients who received allopurinol at first phase, had a significant decrease in the positive, general and total PANSS scores at the sixth month compared with the beginning of the study. It seems that in the beginning of the study, PANSS scores in this group were higher compared with group starting on placebo. This difference wasn’t statistically significant (probably because of low sample size); therefore, despite of significant decrease in patients who received allopurinol at first, there was no significant difference between the two treatments.
After cross-over, the PANSS mean scores decreased in both allopurinol and placebo treatments but it wasn’t statistically significant. Other studies had shown a significant decrease in PANSS mean scores especially for positive and general symptoms in allopurinol treatment.
7,8 Despite no significant difference in our results between two groups, our results are relatively near to other studies7,8 and the possible effect of allopurinol on schizophrenia symptoms is considerable in our study.In our study no response to treatment with two different antipsychotic in doses equivalent with chlorpromazine 1000 mg daily is considered as treatment refraction, while, in other studies the equivalent dose were chlorpromazine 400mg.
7,8 Perhaps the cause of no significant decrease in PANSS scores after intervention is related to high grade of refractoriness of our patients.In this study one year after stopping the treatment with allopurinol and placebo, the positive, negative, general and total PANSS mean score have decreased compared with the beginning of the study. There was a significant difference for negative, general and total symptoms in both groups. It seems that long term use of allopurinol as an augmentation therapy is possibly more effective in schizophrenia patients who are resistant to treatment, but additional studies are necessary to confirm these observations.
Although the daily dose of allopurinol in our study was 600 mg but patients’ tolerance against its side effect was appropriate, except one case that experienced loss of consciousness and was excluded from the study. In this case, we couldn’t relate the event to allopurinol. In our study there was no side effect like skin rash, leukocytosis, eosinophillia, and increase of aminotransferases, that was reported in some earlier study,
10 after treatment with allopurinl. Two previous studies have also not reported serious side effects for allopurinol treatment.7,8There is a lot of evidence showing antagonistic effect of adenosine and dopamine in CNS and interactions between dopamine (D2) and adenosine (A2A) receptors
11 and based on these evidences, previous studies investigated the effect of allopurinol as an augmentation treatment in refractory schizophrenia and positive results have been reported.7,8Our study shows some degree of decrease in symptoms scores. It seems that small sample size and rigid definition of treatment resistant schizophrenia are among the limitations of our study.
CONCLUSION
In conclusion, our study shows some degree of decrease (but not significant) in symptoms scores. More studies with a larger sample size, different doses of allopurinol and different group of patients are necessary in schizophrenic patients.
ACKNOWLEDGMENTS
This study was funded by Kurdistan University of Medical Sciences Vice Chancellor for research. We are grateful to Dr.Karimidostan, Mr. Esfandiari and Mr. Shahsavari and staffs of the chronic caring center, Bahar, in Sanandaj.
REFERENCES
1. Lara DR. Inhibitory deficit in schizophrenia is not necessarily a GABAergic deficit. Cell Mol Neurobiol 2002;22(3):239-47.
2. Mohammadi MR, Akhondzadeh S. Schizophrenia: etiology and pharmacotherapy. IDrugs 2001;4(10):1167-72.
3. Dunwiddie TV, Masino SA. The role and regulation of adenosine in the central nervous system. Annu Rev Neurosci 2001;24:31-55.
4. Machado-Vieira R, Lara DR, Souza DO, Kapczinski F. Therapeutic efficacy of allopurinol in mania associated with hyperuricemia. J Clin Psychopharmacol 2001;21(6):621-2.
5. Lara DR, Cruz MR, Xavier F, Souza DO, Moriguchi EH. Allopurinol for the treatment of aggressive behaviour in patients with dementia. Int Clin Psychopharmacol 2003;18(1):53-5.
6. Lara DR, Brunstein MG, Ghisolfi ES, Lobato MI, Belmonte-de-Abreu P, Souza DO. Allopurinol augmentation for poorly responsive schizophrenia. Int Clin Psychopharmacol 2001;16(4):235-7.
7. Brunstein MG, Ghisolfi ES, Ramos FL, Lara DR. A clinical trial of adjuvant allopurinol therapy for moderately refractory schizophrenia. J Clin Psychiatry 2005;66(2):213-9.
8. Akhondzadeh S, Safarcherati A, Amini H. Beneficial antipsychotic effects of allopurinol as add-on therapy for schizophrenia: a double blind, randomized and placebo controlled trial. Prog Neuropsychopharmacol Biol Psychiatry 2005;29(2):253-9.
9. Wirshing DA, Marshall BD Jr, Green MF, Mintz J, Marder SR, Wirshing WC. Risperidone in treatment-refractory schizophrenia. Am J Psychiatry 1999;156(9):1374-9.
10. Roberts LJ II, Morrow JD. Analgesic-antipyretic and anti-inflammatory agents and drugs employed in the treatment of gout. In: Hardman JG, Limbird LE, Gilman AG, eds. Goodman & Gilman,s The Pharmacological Basis of Therapeutics, Tenth Edition. New York, NY: McGraw-Hill; 2001;687-731.
11. Ferré S, Quiroz C, Woods AS, Cunha R, Popoli P, Ciruela F. An update on adenosine A2A-dopamine D2 receptor interactions: implications for the function of G protein-coupled receptors. Curr Pharm Des 2008;14(15):1468-74.
HOME | SEARCH | CURRENT ISSUE | PAST ISSUES
Professional
Medical Publications
Room No. 522, 5th Floor, Panorama Centre
Building No. 2, P.O. Box 8766, Saddar, Karachi - Pakistan.
Phones : 5688791, 5689285 Fax : 5689860
pjms@pjms.com.pk